Esophageal Diseases
What are esophageal diseases?
What are the types of esophageal diseases?
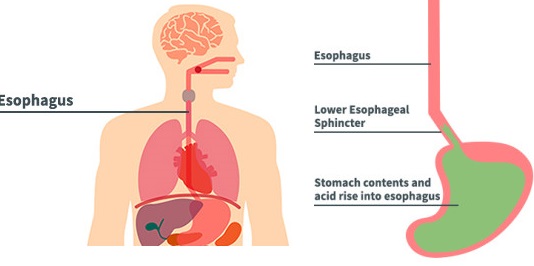
1. GERD:
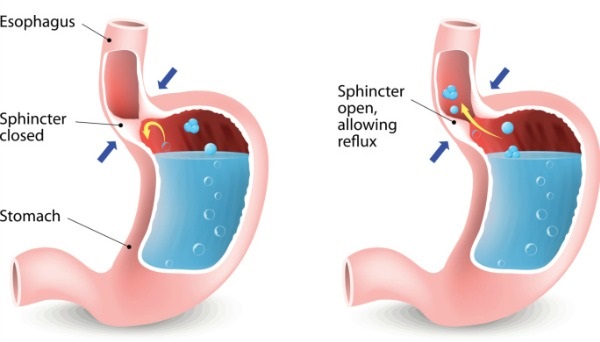
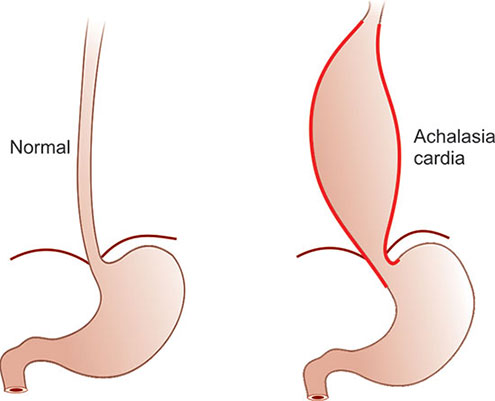
2. Achalasia:
Food cannot enter the stomach because the lower esophageal sphincter is closed or in a relaxed state. Although the precise etiology of achalasia is unknown, experts speculate that it may be an autoimmune condition. Something is causing harm to the nerves that regulate the esophageal muscles.
3. Barrett’s esophagus:
The bottom lining of the esophagus begins to resemble the lining of the stomach in patients with chronic, untreated acid reflux, and the cells begin to resemble intestinal cells. These alterations occur at the junction of the stomach and esophagus. The disease in question is linked to an increased risk of esophageal cancer.
4. Eosinophilic esophagitis:
In this condition, within esophagus, white blood cells known as eosinophils proliferate excessively. Esophagitis, or inflammation of the lining of the esophagus, is the outcome. Patients with various allergies are more likely to have this problem.
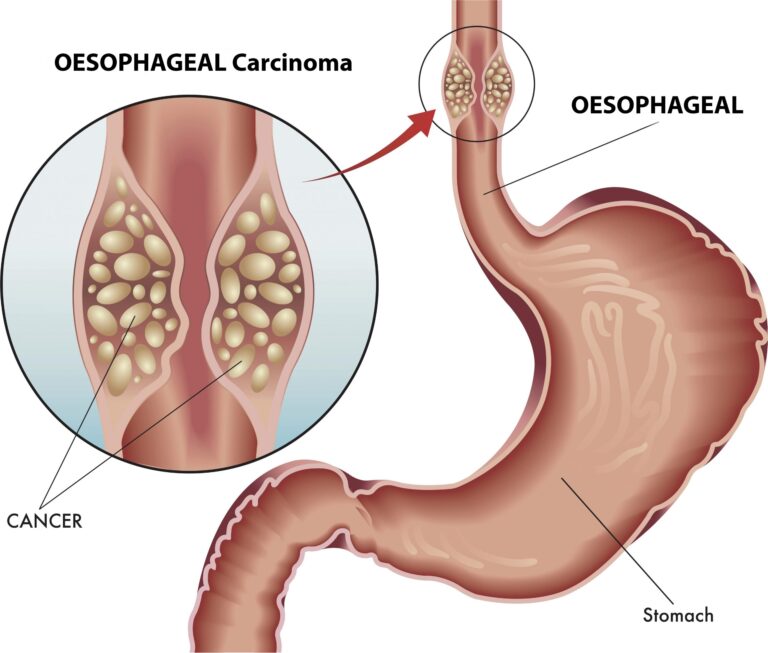
5. Esophageal cancer:
Esophageal cancer can be classified as either adenocarcinoma or squamous cell carcinoma. In general, the risk of esophageal squamous cell carcinoma is increased by smoking, radiation, and HPV infection; the risk of adenocarcinoma is increased by smoking and acid reflux.
Esophageal diverticulum:
Esophageal Injury:
tear like Malloery Weiss tear (incomplete tears happening after vigorous vomiting or retching) or full perforations (punctures or ruptures) can be serious and life threatening injuries. Caustic injuries happen after acid or alkali ingestion by mistake or in suicidal attempts.
Esophageal spasms:
Esophageal spasms are abnormalities of the muscles. This causes difficulty in swallowing with pain.
Esophageal strictures:
In this condition the esophagus narrows excessively, causing difficulty in passage of liquids and food.
Hiatal hernias:
The upper portion of the stomach rests in the chest and protrudes above a diaphragmatic aperture. This illness makes acid reflux worse.
Symptoms of Esophageal diseases:
- Abdominal pain, chest pain or back pain
- Long standing (Chronic) cough or sore throat
- Difficulty in swallowing (Dysphagia), feeling of something stuck in throat (Globus sensation)
- Heartburn (retrosternal, behind the breast bone burning)
- Change in voice (Hoarseness), Wheezing ( also sometimes wrongly diagnosed as asthama)
- Regurgitation or reflux of food or gastric acid
- Unintentional and unexplained weight loss
Risk factors
- Alcohol abuse
- Excess weight and obesity
- Certain medications
- Radiation
- Smoking ( active or passive)
Diagnostic tests
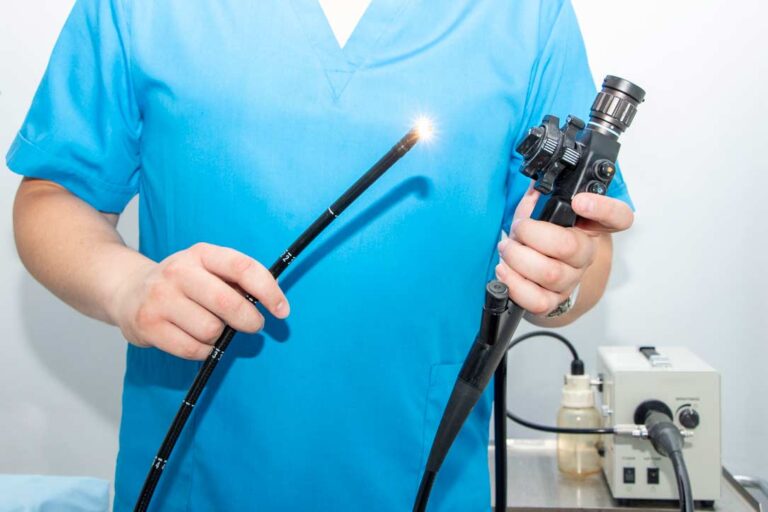
Upper Gastrointestinal / OGD scopy
is a camera on flexible tube passed through the mouth under sedation or local anesthesia which can assess esophagus, stomach and initial part of small intestine. This can also aid in some therapeutic treatments and investigations like biopsy.
Gastrointestinal Xrays
(Barium or Gastrograffin study) is a special type of dynamic xrays after drinking the contrast media to assess the motility function and anatomical abnormalities of upper digestive tract.
Esophageal Manometry
is a special tube passed through esophagus which measures pressure changes during dry and wet swallows to guide the clinician about diagnosis and choosing the particular treatment and also allows classification of certain ailments i.e. Chicago Classification for achalasia cardia
Esophageal pH study
is mainly done to assess the amount of acid coming back in food pipe and also its severity by giving readings for full 24 hours, helping in diagnosis of GERD.
Impedence study
is useful for non acid reflux.
Treatment options
Antacids, proton pump inhibitors and histamine receptor (H2) blockers
to reduce stomach acid.
Endoscopic dilation
Botulinum toxin
(Botox®) injections to temporarily stop esophageal spasms or relax the sphincter muscle.
Esophagectomy
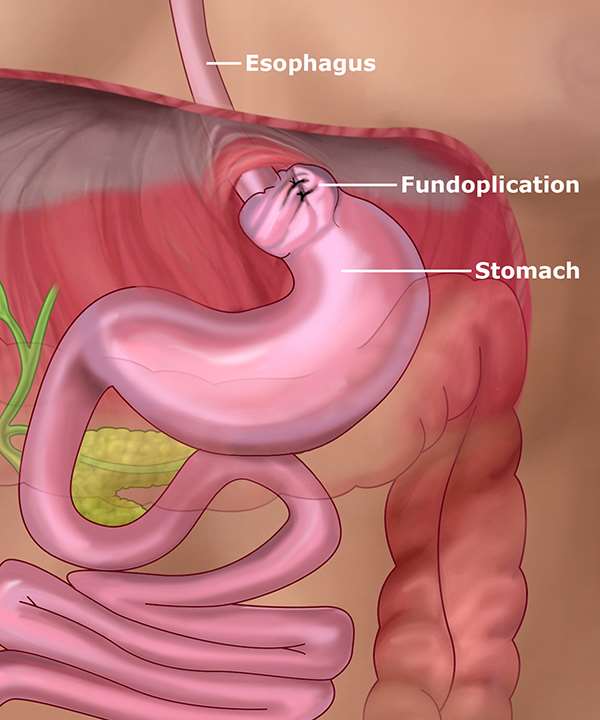
Laparoscopic antireflux surgery (Nissen fundoplication)
Heller myotomy and peroral endoscopic myotomy (POEM)
treat achalasia and esophageal spasms.